Kidneys & Dialysis Education
- Home
- Kidneys & Dialysis Education
Kidneys & Dialysis Education
Your kidneys are about the size of your closed fist. They are located on each side of your spine, under your lower ribs. Although sometimes overlooked, they are just as important to our health as our heart and lungs. To understand what happens when they fail, it’s necessary to first learn how they work.
Your kidneys are the main way that your body cleans toxic waste out of your blood. Every minute, health kidneys take in about 1 liter of blood (about 34 fluid ounces) through the renal arteries. Purified blood is then returned to the rest of the body through the renal veins.
The fluid and wastes collected by the kidneys are sent to the bladder and expelled as urine. Healthy kidneys produce about 2 liters of urine (about 68 fluid ounces) every day. Healthy kidneys are also able to take over for one another – if one fails, the other can compensate.
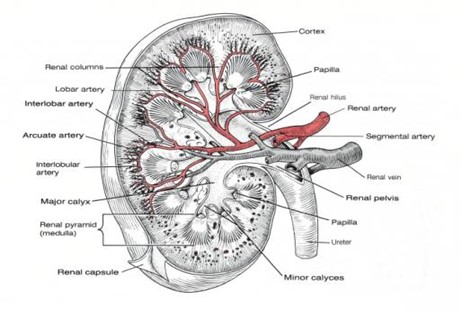
How Kidneys Work
Your kidneys also:
• Regulate water in the body and prevent fluid retention
• Balance essential electrolytes and minerals your cells need
• Produce hormones to regulate blood pressure, make red blood cells, control the body’s absorption of calcium, and manufacture Vitamin D to support bone growth and repair
-
How Kidneys Fail
Kidney failure happens when disease hurts the kidneys’ ability to remove waste from the body.
-
Acute Kidney Failure
Sometimes, people experience a sudden loss of kidney function, coming on within a few hours or days. Kidneys are incredible at healing themselves, so function is nearly always recoverable.
-
Chronic Kidney Failure
A gradual buildup of scar tissue or other problems can result in a slow, gradual loss of kidney function. If kidney function falls to 20% of normal function, serious health problems develop.
-
End Stage Renal Failure
All patients on home and in-center hemodialysis have what is called end stage renal failure. This stage is indicative of total or near total loss of the kidneys ability to rid the body of waste products and to maintain fluid and electrolyte balance. When kidney function falls to 10% or 15% of normal levels, dialysis or a transplant is needed for someone to survive.
Common Causes of Kidney Failure
Diabetes
About 33% of patients with kidney failure have diabetes. Excess glucose (sugar) can cause narrowing of the blood vessels that supply the kidneys. Over time, this can cause damage to the kidneys and result in a gradual buildup of scar tissue.
Polycystic Kidney Disease
This is a hereditary disease that causes the formation of multiple cysts within the kidneys. As these cysts grow, they cause damage to the kidney tissue. It takes time for cysts to grow, so kidney failure does not usually occur until a person is in their 40’s or 50’s.
Immunological Disorders
In this type of kidney disease, the body forms antibodies to fight its own cells and tissues. Some of these diseases cause the formation of antibodies that fight kidney tissue, causing extensive damage. Glomerulonephritis is an example of an immunologic disorder.
High blood pressure
Also called hypertension, high blood pressure can damage the kidneys’ blood vessels and tissue. High blood pressure may either be a cause of kidney failure or may result from kidney disease, but no matter what, it can hasten kidney decline. It damages the small blood vessels delivering blood to the kidneys’ filters by straining and pressing them. Untreated high blood pressure will greatly reduce blood flow into the filters and will result in kidney failure.
Your kidneys also produce a hormone called renin involved in the control of blood pressure. When the kidneys are damaged or fail, this hormone may be produced in large amounts and cause hypertension. In turn, hypertension may lead to further kidney damage. It’s a vicious cycle, and that’s why it’s important to have your blood pressure checked regularly.
Drug-induced Kidney Disease
Some medications can be toxic to kidneys. Exposure to these medications over time can lead to kidney damage. Pain medications and anti-arthritis drugs are the most common offenders. Non-prescription pain killers may damage the kidneys if used in large doses over a long period of time, or if taken without proper hydration during illness (this can result in acute kidney failure).
Signs and Symptoms of Kidney Failure
- High blood pressure
- Protein in the urine
- Blood in the urine
- Tea-colored urine
- Foaming urine
- Change in frequency of urination
- Swollen feet & ankles
- Passing urine at night
- Pain in the back or side
- Itchy skin
- Puffiness around the eyes
- Shortness of breath

What Happens When Kidneys Fail? Fluid, Electrolyte and Mineral Imbalance
When the kidneys fail, uremia occurs. Uremia is a Greek word and means urine in the blood. The signs of uremia occur when 80-85% of normal kidney function is lost. Symptoms of uremia are many and can significantly impact quality of life – if untreated, uremia is ultimately fatal.
Swelling and Shortness of Breath
The ability to get rid of excess fluid is impaired, resulting in swelling and shortness of breath. Swelling usually occurs in the feet, ankles, and around the eyes.
Unstable Blood Pressure
Retention of salt and fluid contributes to high blood pressure. Healthy kidneys produce a hormone called renin, which helps control blood pressure. Diseased kidneys may produce too much renin, which can contribute to high blood pressure.
High Potassium
Regulation of potassium (an electrolyte) which regulates heartbeat and muscle function, is also impaired. High levels of potassium may result in irregular heartbeat and muscle weakness. Extremely high levels of potassium can make the heart stop beating.
Excess Acid in the Blood
The kidneys also regulate the amount of acids in the blood by getting rid of hydrogen and retaining bicarbonate. Excess acid may need to be regulated by medication or dialysis.
Renal Bone Disease
The kidneys play a vital role in regulating levels of calcium, phosphorus, parathyroid hormone, and Vitamin D in the blood. Imbalances in these substances will lead to renal bone disease, a condition associated with bone pain, fractures, and eventually immobility.
Itching
Excessive levels of calcium, phosphorus, and waste products such as urea will cause itchy and irritated skin.
What is Dialysis? Life-Saving Interventions for Severe Kidney Disease
Dialysis is a medical treatment that replicates the function of healthy kidneys when your kidneys are no longer able to work well. It removes waste products, excess fluid, and toxins from the blood when the kidneys can’t and helps conserve your kidneys’ remnant functions.
Types of Home Dialysis
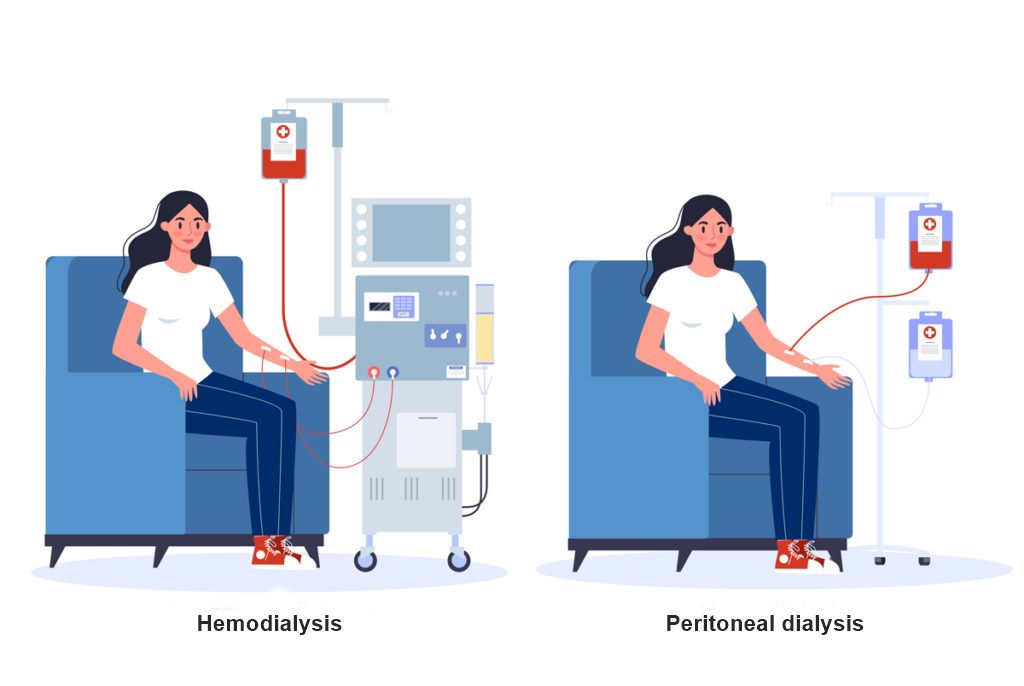
Hemodialysis (HD)
- Conventional Home Hemodialysis: Typically performed three times a week, each session lasting about four to five hours.
- Daily Home Hemodialysis: More frequent dialysis that can lead to better fluid balance and stable blood toxin levels.
- Nocturnal Home Hemodialysis: Performed overnight, allowing for a slower, more extended filtration process similar to your natural kidney function.
Peritoneal Dialysis (PD)
- Continuous Ambulatory Peritoneal Dialysis (CAPD): Manual exchanges several times a day without the need for a machine.
- Automated Peritoneal Dialysis (APD): Uses a machine to perform exchanges usually at night while you sleep.
Choosing the Right Type of Dialysis
Your choice between hemodialysis and peritoneal dialysis often depends on personal preferences, lifestyle, medical condition, and your home situation. Our nephrologists will help you determine the best type of dialysis for your situation based on your overall health, kidney function, and personal needs.
Support and Training
- Safely Operate Dialysis Equipment: Whether at home or elsewhere.
- Manage Treatments: Including how to handle supplies and respond to any issues that may arise during dialysis.
Benefits of Home Dialysis
- Improved Quality of Life: Dialysis can significantly improve your quality of life during advanced kidney disease by removing toxins and balancing fluids.
- Flexibility and Independence: Home dialysis options provide flexibility to maintain a more normal lifestyle, with treatments that can be scheduled around your needs.

Did You Know
Between 2009-2019 The number of patients performing Home Dialysis has nearly doubled from 6.8% to 12.6% of the ESRD population, with growth driven mainly by peritoneal dialysis. More than 90% of Renal professionals would choose home dialysis as the initial treatment option if they were a dialysis patient.
Fluid overload is a common symptom among 3x times weekly in-center hemodialysis patients. This can lead to heart disease from the constant swelling of the heart muscles. 45%-50% of in-center hemodialysis patients die from cardiovascular disease. More frequent hemodialysis, which is offered by in-home options, provides better fluid management and is associated with lower rates of cardiovascular death.